Prescribing Question (10 marks)
Suggested time: 6 minutes.
You are allowed the use of a BNF and a calculator at any time.
Prescribing Question (10 marks)
Suggested time: 6 minutes.
You are allowed the use of a BNF and a calculator at any time.
Case presentation
A 54-year-old lady presents to hospital complaining of a 3 day history of a productive cough and shortness of breath. She is producing green sputum. She is usually fit and healthy and has had no previous symptoms before. PMH. Hypertension. DH. She normally takes Ramipril 2.5mg No allergies. SH. Lives at home on her own. Mobilises without aid and is self-caring.
On examination patient is alert and responsive.
Clinical examination reveals the following signs:
O2 sat 93% on air, BP 113/74mmHg, HR 70/min and regular, JVP within normal limits, HS S1+S2+0, RR 25/min, T 38.2, chest sounds: Crackles over left mid zone and reduced air entry over left base.
Investigations
The results of the available investigations are:
Na+ 137 mmol/L (137–144), K+ 4.0mmol/L (3.5–4.9), U 5.2 mmol/L (2.5–7.0), Cr 100 µmol/L (60–110), HB 12 g/dL (11.5-16), WCC 15 x 10⁹ /L (4-11)-neutrophilia, Plat 345 x 10⁹ g/dL (150-400)
ECG shows sinus tachycardia
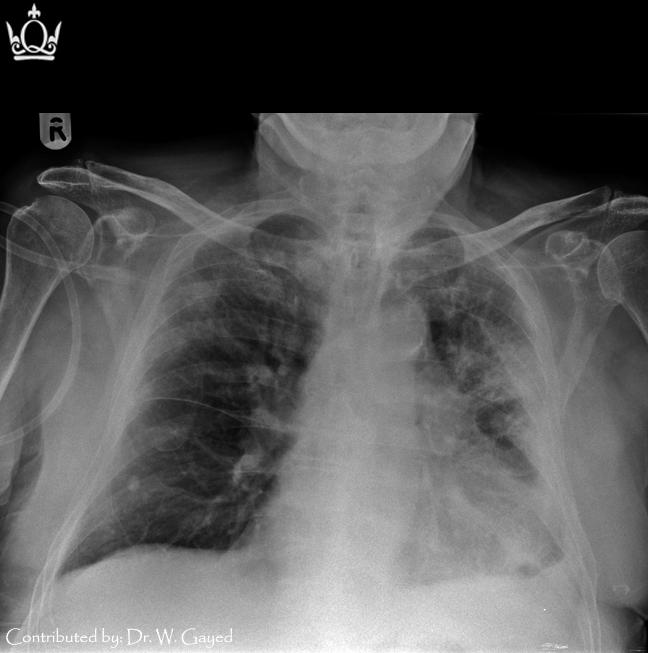
CXR is as illustrated (left)
Teacher's Comment
1) Confusion (Abbreviated Mental Test (AMT) score of 8 or less)
2) Urea >7mmol/L
3) Respiratory rate 30/min
4) Blood pressure (SBP< 90mmHg or DBP 60mmHg)
5) Age 65yrs